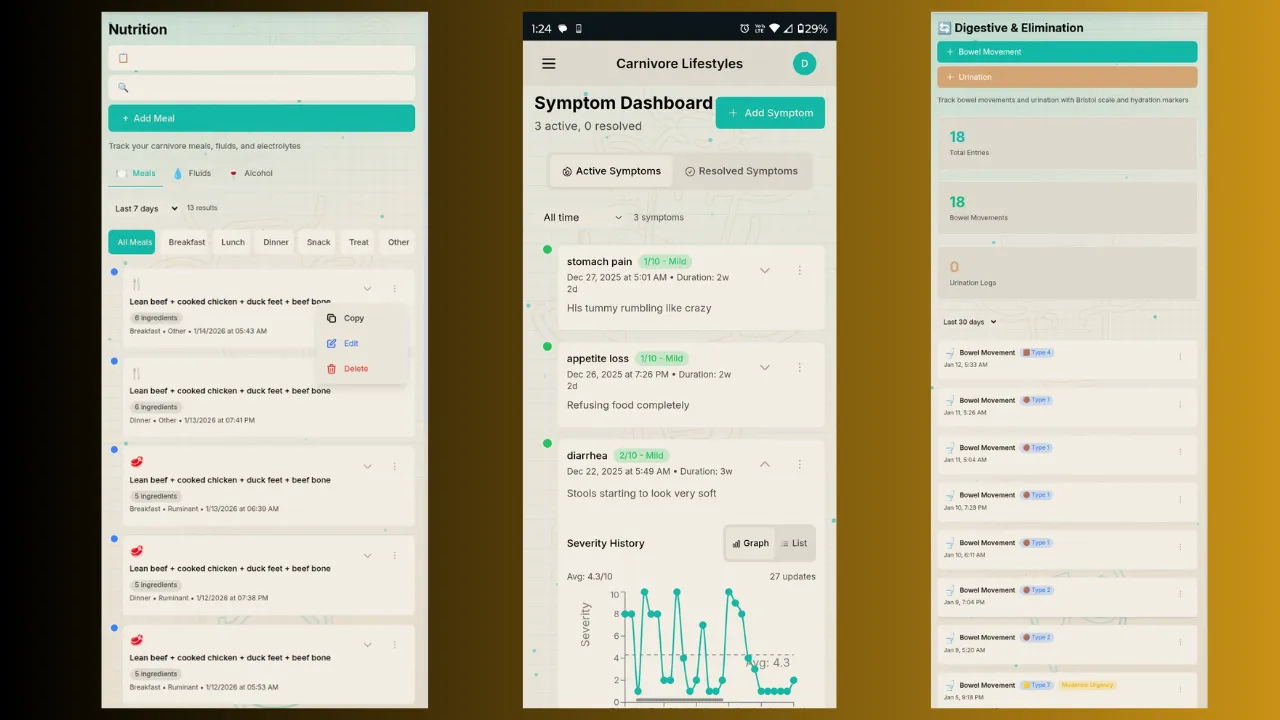
You finally committed to an elimination diet. You cut the foods. You felt better — maybe a lot better. Then you started adding things back, and suddenly symptoms returned. But which food caused it? Was it the eggs you ate yesterday? The dairy from two days ago? Or something else entirely?
This is where most elimination diets fall apart. Not because the approach is wrong — it's actually the gold standard recommended by allergists and gastroenterologists worldwide. It fails because people don't track.
Without consistent tracking, an elimination diet is just... a restrictive diet with no answers.
Quick Facts
- Food sensitivity reactions can be delayed by up to 72 hours — sometimes even longer. That means the food that made you feel terrible on Wednesday might be something you ate on Monday.
- Up to 20% of people worldwide may experience some form of food intolerance or sensitivity, yet most never identify the specific trigger.
- Elimination diets work across all reaction types — immune, enzymatic, chemical, and combination reactions. No blood test can do that.
- Veterinary experts agree: for dogs and cats with suspected food sensitivities, an 8–12 week elimination diet with careful monitoring is the only reliable diagnostic tool. Serum and saliva tests for pets have no scientific backing.
- A 2024 randomised controlled trial found that participants who received structured support and guidance during an elimination diet reported greater adherence and better health outcomes than those who tried to go it alone.
Why Tracking Makes or Breaks Your Results
An elimination diet has two phases: removal and reintroduction. Both depend entirely on your ability to connect what you eat with how you feel.
Here's the catch: food sensitivities don't play fair. Unlike a true allergy (think hives within minutes of eating peanuts), sensitivities are sneaky. Reactions can show up hours or even days after you eat a trigger food. They can also be dose-dependent — a little bit might be fine, but eat that same food three days in a row and symptoms flare.
Without a written record, your brain simply cannot hold all the variables. You'll forget what you ate on Tuesday. You'll misattribute Thursday's headache to stress instead of the cheese you reintroduced two days earlier.
Tracking turns guesswork into data. And data gives you real answers.
What to Track (and Why Each One Matters)
You don't need to write a novel every day. But the more consistently you log a few key things, the clearer your picture becomes.
- Everything you eat and drink — including exact ingredients, cooking methods, and portion sizes. "Salad" isn't enough; you need to know what was in the salad.
- Time of each meal and snack — this helps link symptoms to specific meals when reactions are delayed.
- All symptoms, with severity — rate them on a simple 1–10 scale. Note when they started and how long they lasted.
- Sleep quality and duration — poor sleep can amplify food reactions and mimic sensitivity symptoms.
- Stress levels — stress directly affects gut function and immune regulation. A stressful week can make a tolerated food suddenly problematic.
- Bowel movements — changes in frequency, consistency, and comfort are early signals.
- Energy levels throughout the day — fatigue patterns often reveal food connections before other symptoms do.
- For pets: track food (exact protein, brand, any treats), scratching/licking behaviour, ear condition, stool quality, energy, and any supplements or medications.
How Symptoms Show Up — Humans vs. Pets
One reason tracking matters so much is that symptoms look very different depending on who's affected.
In humans: Often gut issues (bloating, IBS-like symptoms), skin rashes/psoriasis, joint pain, fatigue, brain fog, headaches, or mood changes.
In pets (mostly dogs and cats): Usually skin first — constant itching, licking paws/face/ears/rear, red skin, ear infections, hot spots, hair loss. Gut signs (vomiting, diarrhoea, gas) happen but are less common than in people.
Severe shock reactions (like anaphylaxis) are rare in pets.
In both humans and pets, these symptoms can take days or even weeks to fully appear after exposure to a trigger food. That's exactly why a one-time observation isn't enough — you need a running log to spot delayed patterns.
What Tracking Reveals That No Test Can
A blood test gives you a single snapshot. Tracking gives you a living dataset that captures how your body actually responds over time. Here's what consistent tracking can uncover:
- Delayed reactions that appear 24–72 hours (or more) after eating a trigger
- Cumulative effects — small amounts are fine, but repeated exposure over several days triggers symptoms
- Contextual triggers — stress, hormonal cycles, poor sleep, or illness that amplify food reactions
- Changing sensitivities — as your gut heals, some triggers may resolve while new ones can emerge
- Combination effects — two individually tolerated foods eaten together cause a reaction
No lab panel can capture this level of personal detail. Your body is, quite literally, the most accurate lab you have.
How Long Should You Track?
This is where patience becomes your best friend.
- Elimination phase: Most practitioners recommend 2–4 weeks for humans. For pets, the gold standard is 8–12 weeks of a strict novel-protein diet.
- Reintroduction phase: Add one food back at a time. While some guidelines suggest a minimum of 3 days between foods, many practitioners recommend eating the reintroduced food for 1–2 weeks before drawing conclusions. Why? Because some sensitivities are dose-dependent and cumulative — a small amount on day one might feel fine, but eating that same food daily for a week can push you past your body's threshold and trigger a reaction. For pets, veterinary dermatologists recommend 1–2 weeks per food during the challenge phase. Go slow. Track carefully throughout.
- Meaningful AI or pattern analysis typically requires 45–60 days of consistent data to reveal reliable food-symptom connections, especially delayed ones.
It took one pet owner over 9 months to fully resolve her dog's itching and yeast issues — and tracking was what finally revealed which proteins were safe and which were not. These things take time. But without the data, that time is wasted. For dedicated pet tracking resources, see ItchyPet.
Tips to Make Tracking Stick
- Keep it simple. Two minutes a day is enough if you're consistent. Don't aim for perfection — aim for consistency.
- Log in real time. Don't try to remember at the end of the day. Note meals and symptoms as they happen.
- Use a dedicated tool. Spreadsheets, journals, and apps all work. What matters is having everything in one place so patterns can emerge.
- Track even on "good" days. Knowing what you ate when you felt great is just as valuable as knowing what caused a flare.
- Share your data. Bring your log to your practitioner, dietitian, or vet. Clinicians consistently report that patient food diaries make appointments more focused and productive.
The Bottom Line
An elimination diet without tracking is like running an experiment without writing down the results. You might feel better during the elimination phase, but you'll struggle to identify exactly which foods are your friends and which are your foes.
Tracking is what transforms a restrictive diet into a powerful diagnostic tool — for you, your family, and your pets.
The delayed nature of food sensitivity reactions makes it nearly impossible to rely on memory alone. But with consistent, structured tracking — even just a few minutes a day — you can uncover patterns that no blood test, no guesswork, and no amount of Googling will ever reveal.
Start tracking. Be patient. And if you need guidance, consult a holistic practitioner or integrative vet who understands elimination diets and can help you read the data your body is already giving you.
Your body has the answers. Tracking is how you hear them.
Data Sources
1. Malone JC, Daley SF. Elimination Diets. StatPearls. Updated January 9, 2024. National Library of Medicine.
2. Tuck CJ, et al. Food Intolerances. Nutrients. 2019;11(7):1684. PMC.
3. D'Adamo CR, et al. Functional medicine health coaching improved elimination diet compliance and patient-reported health outcomes. Medicine (Baltimore). 2024;103(8):e37148.
4. Stapel SO, et al. Testing for IgG4 against foods is not recommended as a diagnostic tool: EAACI Task Force Report. Allergy. 2008;63(7):793–796.
5. Carr S, et al. CSACI Position statement on the testing of food-specific IgG. Allergy Asthma Clin Immunol. 2012;8(1):12.
6. Lomer MCE. The 2023 BSG guidelines on diet and IBS. Gut. 2023.
7. Coyner K, Schick A. Hair and saliva test fails to identify allergies in dogs. J Small Anim Pract. 2019;60(2):121–125.
8. Olivry T, Mueller R, Prélaud P. Critically appraised topic on adverse food reactions of companion animals (1): duration of elimination diets. BMC Vet Res. 2015;11:225.
9. Vandre Clear. Elimination diet trials for dogs and cats. Royal Canin Academy. 2024.
10. Raman R. How to Do an Elimination Diet and Why. Healthline. Updated December 2024.
11. Tham HL. Elimination Diet Trials: Steps for Success and Common Mistakes. Today's Veterinary Practice. 2024.
12. 5 Common Elimination Diet Trial Mistakes. Today's Veterinary Nurse. 2024.
13. IFN Academy. Addressing Adverse Food Reactions: A Functional Nutrition Approach. 2025. (Type II/III reactions are dose-dependent; repeated exposure creates cumulative hypersensitivity.)
14. Wikipedia contributors. Food Intolerance. Wikipedia. Updated 2025. (Non-allergic food reactions can be delayed, dose-dependent, and cumulative across exposures.)
15. Monash University. Low FODMAP Diet Reintroduction Protocol. (Recommends approximately one week per FODMAP group during reintroduction testing.)
Medical disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before making changes to your diet or discontinuing any prescribed treatments. If you suspect a true food allergy (especially one causing severe or anaphylactic reactions), seek evaluation from a board-certified allergist.