This article is written in Kristina's voice — the founder of Carnivore Lifestyles, competitive ocean racer, and 25-year psoriasis veteran.
I've been managing psoriasis since my early twenties. Twenty-five years of plaques, flares, remissions, and the particular exhaustion that comes from never quite knowing what's coming next. I've done the steroid creams, the light therapy, the restrictive protocols, the expensive supplements. I've been told it's genetic (true), autoimmune (also true), stress-related (partially true), and — my personal favourite — something I just have to "manage."
What nobody told me for the first two decades was that the food I was eating was doing a significant part of the damage. Not because food causes psoriasis — it doesn't. But because specific foods were triggering the inflammatory cascade that drove my flares. And the reason I didn't know was simple: the reactions were delayed.
The Pattern I Could Never See
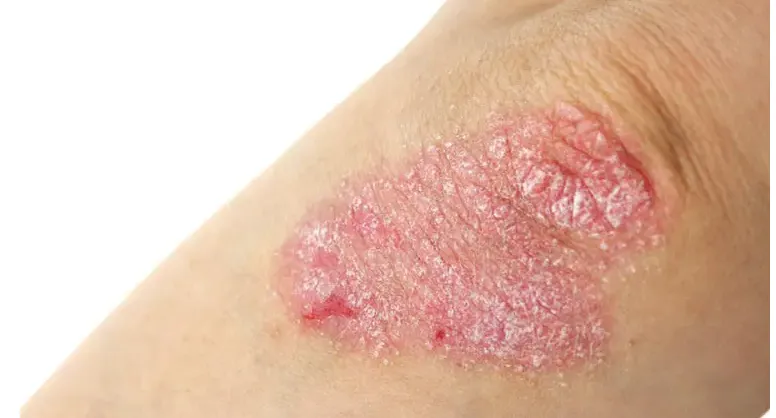
Psoriasis is an autoimmune condition. The immune system misfires and causes skin cells to multiply at an accelerated rate, producing the raised, silvery plaques most people recognise. In people with psoriasis, the immune system is already primed to overreact — which means anything that adds to the inflammatory load can tip the balance and trigger a flare.
For years, I tracked everything except the one thing that mattered most: the connection between what I ate and when my skin changed.
I noticed patterns in a vague, imprecise way. "I always seem to flare when I'm stressed" — true, but incomplete. "I had a bad winter this year" — also true, but not the whole story. What I couldn't see was that underneath the stress and the seasonal variation, there were repeating dietary triggers that were amplifying every flare.
The problem isn't that the pattern doesn't exist. It's that the human brain, unaided, cannot hold the volume of data required to see it. You don't remember what you ate on Tuesday when your skin erupts on Saturday. You blame the Saturday stress, the Saturday weather, the Saturday anything.
What Changed When I Started Tracking
The first time anyone connected food to my flares was about ten years ago, at a clinic in Melbourne. They told me to avoid nightshades and a handful of other components. I followed the protocol, and it worked — initially. My skin improved noticeably, and I assumed I'd found the answer.
But over the years, I drifted. I started eating "healthier" — which, at the time, meant adding more and more vegetables to my diet. By 2022, the more plant-forward I ate, the worse my skin seemed to get. The nightshade avoidance alone wasn't enough anymore, and I couldn't work out why. I was doing everything "right" and getting worse.
In 2023, I tried carnivore for the first time. And when I paired the dietary change with consistent, daily tracking — meals, symptoms, severity, sleep, stress, exercise — the picture started to emerge over weeks.
Some things I suspected were confirmed: periods of high stress did correlate with flares. But the food patterns were the revelation. The green leafy vegetables I'd been loading up on — because I thought eating more of them was "healthier" — were appearing consistently in the 3–5 days before my worst flares. Not every time. But enough times that the data made it undeniable.
When I removed those foods from my diet, something I had not experienced in years happened: a stretch of genuinely clear skin. Not improved. Clear.
But the story didn't end there. My skin cleared up — and then my athletic performance tanked. Carnivore gave me the cleanest skin I'd had in decades, but my body needed more to sustain international-level ocean racing. And now, going through age-related hormonal changes, the triggers have shifted once again. What worked two years ago doesn't work the same way today.
That's the part nobody tells you about elimination diets: they're not a one-time fix. Your body changes. Your triggers change. The only constant is that without ongoing tracking, you're guessing — and guessing is what got most of us into trouble in the first place.
The Foods Most Commonly Linked to Psoriasis Flares
Research on diet and psoriasis is growing, though the evidence base is still developing. What's becoming clearer is that psoriasis shares inflammatory pathways with other autoimmune and metabolic conditions, which means the same dietary factors that drive systemic inflammation generally can amplify psoriatic activity specifically.
Alcohol — There is strong evidence that alcohol worsens psoriasis severity. It increases gut permeability, disrupts immune regulation, and may directly amplify the Th17 immune pathway involved in psoriasis. This is one of the most robustly supported dietary connections.
Refined carbohydrates and sugar — High glycaemic diets drive insulin spikes and promote the production of pro-inflammatory cytokines. Research suggests that obesity and metabolic dysfunction worsen psoriasis, and diet is a significant driver of both.
Gluten — The relationship between psoriasis and gluten is complicated and individual. Studies have found elevated anti-gliadin antibodies in a subgroup of people with psoriasis, and some patients see improvement on a gluten-free diet. For others, gluten appears to be a non-issue. Tracking is how you find out which group you're in.
High-histamine foods — Aged meats, smoked fish, vinegar, fermented products, and certain processed foods contain histamine that the body must break down. In people with reduced diamine oxidase (DAO) activity — which may be more common in those with autoimmune conditions — histamine accumulates and can drive systemic inflammation.
Nightshades — Tomatoes, peppers, aubergines, and potatoes contain alkaloids (solanine, capsaicin) that some people with autoimmune conditions find inflammatory. The evidence here is largely anecdotal, but the pattern appears consistently enough in tracking data that it's worth testing individually.
Dairy — Specifically casein and whey proteins, which can drive immune activation in sensitive individuals and are worth eliminating during a baseline phase.
What none of this tells you is which of these — if any — are relevant to you. Psoriasis is not a monolithic condition. It sits on a spectrum of severity and is influenced by a unique combination of genetics, gut health, stress patterns, and lifestyle factors. Your triggers will not look exactly like mine.
Why the Carnivore Approach Works as an Elimination Baseline
What I didn't understand at first was why carnivore worked so dramatically for my skin. It wasn't that meat was healing me — it was that by eating only well-tolerated animal foods, I'd stripped out virtually every common dietary trigger for inflammatory conditions in one step. Gluten, plant antinutrients, histamine-heavy processed foods, refined carbohydrates — all gone. My body finally had a chance to calm down.
That's what makes the carnivore approach so effective as an elimination baseline. You're not guessing which category of food to cut — you're removing the entire field and starting from a clean slate.
From that baseline, the real work begins: systematic reintroduction, one food category at a time, tracked carefully over days and weeks. That's when you build your personal food map — not mine, not a protocol's, yours.
What Systematic Tracking Makes Possible for Psoriasis
The goal is not to find a permanent, static diet you follow forever. It's to understand your body's unique reactivity well enough to make informed decisions — and to notice when things are changing.
Tracking for psoriasis management specifically should include:
- Meals — exact foods, timing, quantities
- Skin condition daily — severity of plaques, new spots, itching intensity, on a 1–10 scale
- Sleep quality — poor sleep directly worsens psoriasis via cortisol and inflammatory pathways
- Stress level — a necessary confound variable. Without tracking it, you can't separate a stress flare from a food flare
- Exercise and recovery — intense exercise temporarily elevates inflammation; knowing your pattern helps interpret symptom data
- Bowel regularity — gut health and skin health are intimately connected in autoimmune skin conditions
- Alcohol — even small amounts can amplify psoriasis in sensitive individuals; tracking this eliminates a major confound
After approximately 45–60 days of consistent data, patterns start to emerge clearly enough for AI analysis to surface connections — including delayed ones spanning 3–5 days — that are impossible to spot manually.
Your Dog May Be Showing You the Same Signal
If you have a dog alongside your own psoriasis or autoimmune journey, you may be managing two different expressions of the same underlying problem: chronic inflammation driven by dietary triggers that the body can't clear efficiently.
DJ and Shadow came into my life after I'd already started my own tracking journey. But when DJ's pancreatitis attacks started — terrifying, expensive, 2am-emergency-level events — I recognised the same pattern: food-triggered inflammation, with specific triggers that took months of tracking to isolate precisely. Shadow's cancer management depends on eating the right proteins for his immune system to function optimally.
Tracking for all three of us — myself, DJ, and Shadow — is ultimately what inspired me to build Carnivore Lifestyles. What I discovered — and what many of our members discover — is that the family that tracks together heals together. Managing your own elimination diet is easier when you're already in the tracking habit. And if your dog has recurring skin problems, gut issues, or unexplained behavioural changes, the cause is often the same family of triggers: dietary proteins their system can't tolerate.
One account. Every human and every pet. All the data in one place.
If you're managing a dog with skin issues or food sensitivities, ItchyPet has resources built specifically for pet food sensitivity tracking.
Twenty-Five Years Later
I'm not going to tell you that tracking cured my psoriasis. It hasn't. What it's done is give me back control over something that felt completely random for most of my adult life.
I know now which foods reliably worsen my skin. I know the lag time between exposure and flare in my own body. I know which environmental and lifestyle factors amplify a food reaction, and which protect against it. I can walk into a stressful month knowing I need to be stricter about my food choices, because I've seen that interaction in my own data.
That knowledge — personal, specific, earned through consistent tracking — is worth more to me than any protocol someone else designed for a body that isn't mine.
If you've spent years guessing, it might be time to try knowing.
Data Sources
Armstrong AW, Read C. Pathophysiology, Clinical Presentation, and Treatment of Psoriasis: A Review. JAMA. 2020;323(19):1945–1960.
Qureshi AA, Dominguez PL, Choi HK, Han J, Curhan G. Alcohol intake and risk of incident psoriasis in US women: a prospective study. Arch Dermatol. 2010;146(12):1364–1369.
Barrea L, et al. Nutrition and psoriasis: is there any association between the severity of the disease and adherence to the Mediterranean diet? J Transl Med. 2015;13:18.
Kolchak NA, et al. Prevalence of antigliadin IgA antibodies in psoriasis vulgaris and response of seropositive patients to a gluten-free diet. J Am Acad Dermatol. 2018;78(4):683–690.e1.
Maintz L, Novak N. Histamine and histamine intolerance. Am J Clin Nutr. 2007;85(5):1185–1196.
Simopoulos AP. The importance of the ratio of omega-6/omega-3 essential fatty acids. Biomed Pharmacother. 2002;56(8):365–379.
Fasano A. Zonulin and its regulation of intestinal barrier function: the biological door to inflammation, autoimmunity, and cancer. Physiol Rev. 2011;91(1):151–175.
Mu Q, Kirby J, Reilly CM, Luo XM. Leaky gut as a danger signal for autoimmune diseases. Front Immunol. 2017;8:598.
Malone JC, Daley SF. Elimination Diets. StatPearls. Updated January 9, 2024.
Medical disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional before making changes to your diet or discontinuing any prescribed treatments. Psoriasis is a complex autoimmune condition — if you are currently managed with immunosuppressant or biologic medication, do not alter your treatment plan without direct guidance from your dermatologist or rheumatologist. If you suspect a true food allergy (especially one causing severe or anaphylactic reactions), seek evaluation from a board-certified allergist.